Better access. Better quality. Better outcomes for your members.
Joy partners with health plans to expand primary care access, close care gaps, and improve quality metrics — with measurable, accountable results.
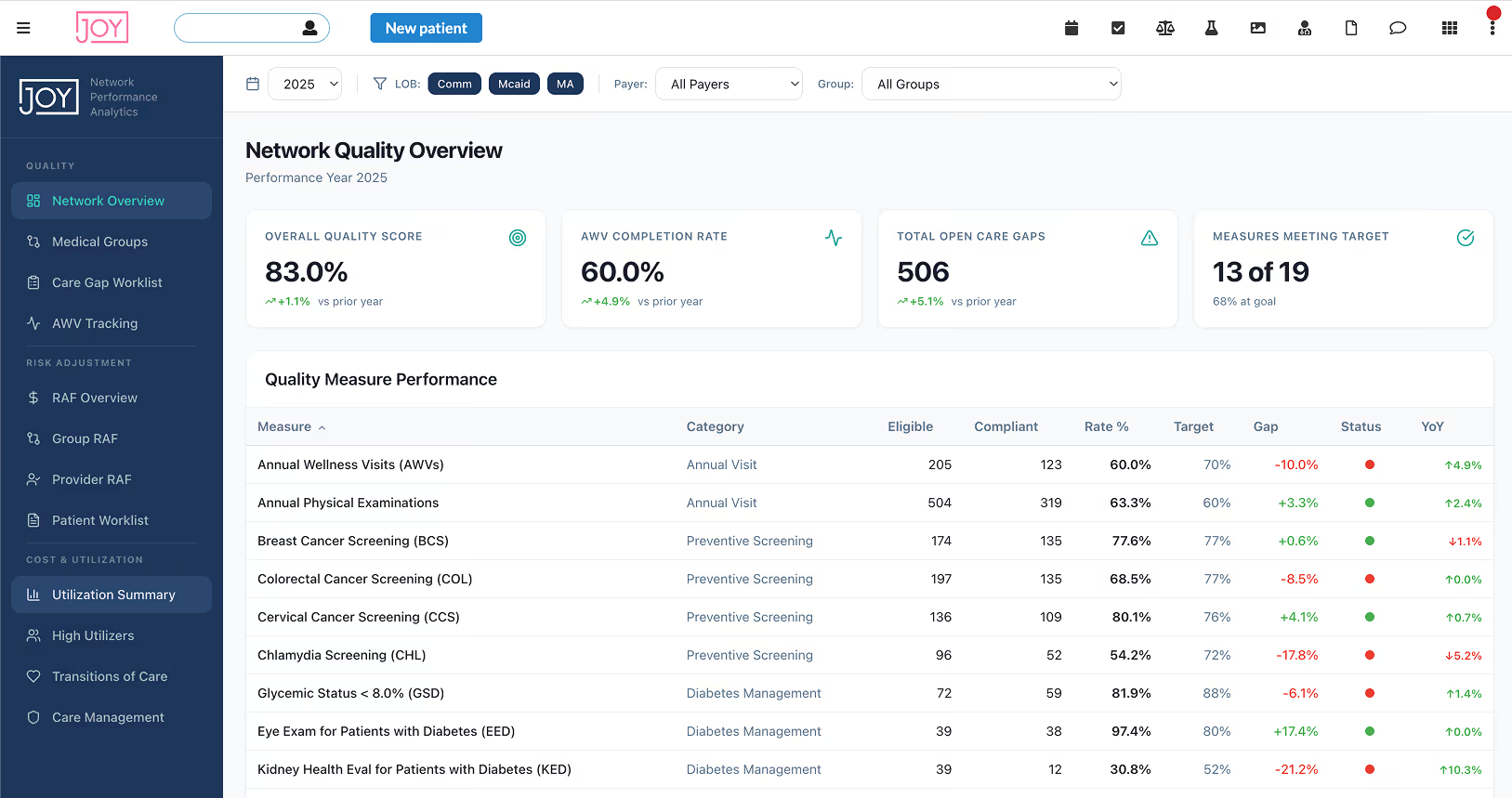
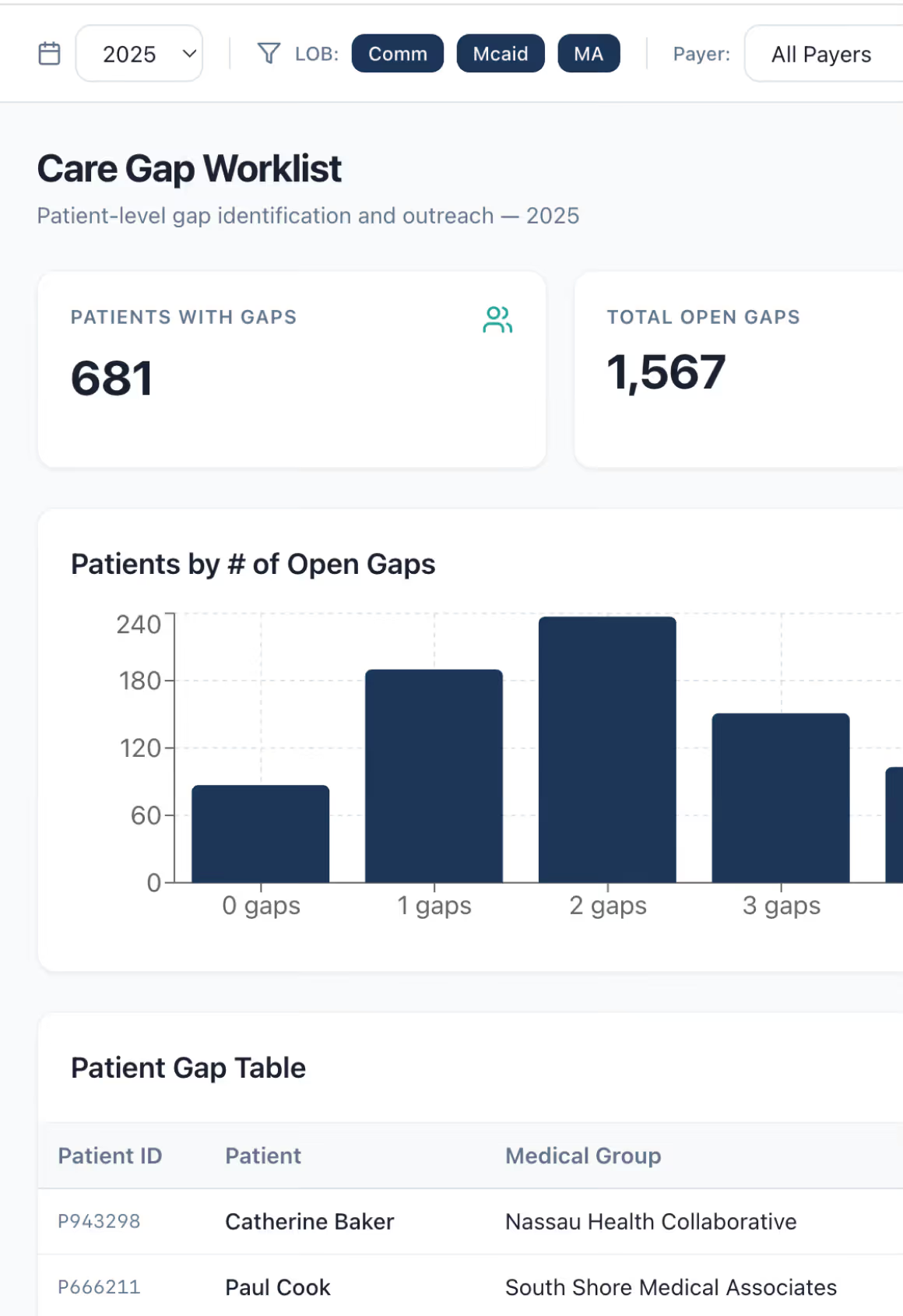

Your members can't get in to see a PCP. Your HEDIS and Stars scores are leaving money on the table. Your provider network has gaps in coverage and quality that analytics alone can't fix. You need a partner that doesn't just identify problems — one that solves them.
What Joy delivers for your plan
Joy handles the operational burden of deploying primary care where it's needed most. You get new capacity, better quality scores, and a partner whose success depends on yours.
Expand network access
Joy launches NP-led practices in underserved markets, adding new access points for your members. Each practice is credentialed with your plan and designed to accept your membership from day one.
Drive quality and Stars performance
Joy's Population Health Services deploy clinical teams to drive Annual Wellness Visits, close HEDIS gaps, improve clinical documentation, and boost member engagement — directly impacting your quality scores and bonus potential.
Accountable partnership
Joy doesn't sell software licenses. We deliver outcomes. Our model aligns financial incentives with yours — we succeed when your members are healthier, your quality scores improve, and your network performs.
Let's talk about your markets.
Ready to move the needle on quality and access?
